We are a trusted billing company known for maximizing reimbursements and reducing claim errors through advanced automation and specialty-specific billing expertise.
Started On
Review Period
Collection Increased
Revenue Increased by
We are a trusted billing company known for maximizing reimbursements and reducing claim errors through advanced automation and specialty-specific billing expertise.

What sets us apart from our competitors is our ability to scale healthcare revenue cycle management solutions around your practice needs. When we pitch you our RCM, we actually start from the past and look at what you still owe that's overdue in billing and claims, and that's where we know where to bring improvements. Then we come up with solutions that help you be more efficient in collecting. Strategic AR recovery plays a crucial role in maximizing revenue by ensuring that healthcare providers collect the maximum amount possible from their services.

Our healthcare revenue cycle management services span over 50+ specialties. Whether managing complex cardiology procedures, pain management therapies, dermatology codes, or mental health payer requirements, we deliver results. No matter what medical billing field you're in or what practice you belong to, we analyze the specific inefficiencies in your operations and provide tailored solutions. This approach enables us to streamline your billing processes and improve overall financial performance.
Our physicians medical billing services deliver complete lifecycle billing management—from charge capture to denial follow-ups—customized to your specialty and size of practice.
For a detailed guide, please explore the following video:

Reduce overhead expenses by 50% and eliminate the need for an in-house team through our efficient physician billing solutions.
Our physician billing services are fully compliant with HIPAA protocols. We stay up-to-date with the latest regulatory standards so that there are no chances of errors or penalties
Our expert billing and coding team submits all claims electronically within 72 hours. We vigorously track every claim and ensure that you get the maximum reimbursements from your payers. We utilize real-time claim scrubbers and payer-specific rules engines to reduce rejections.
To learn more about our services, please fill out the form below and we will be happy to get back to you.
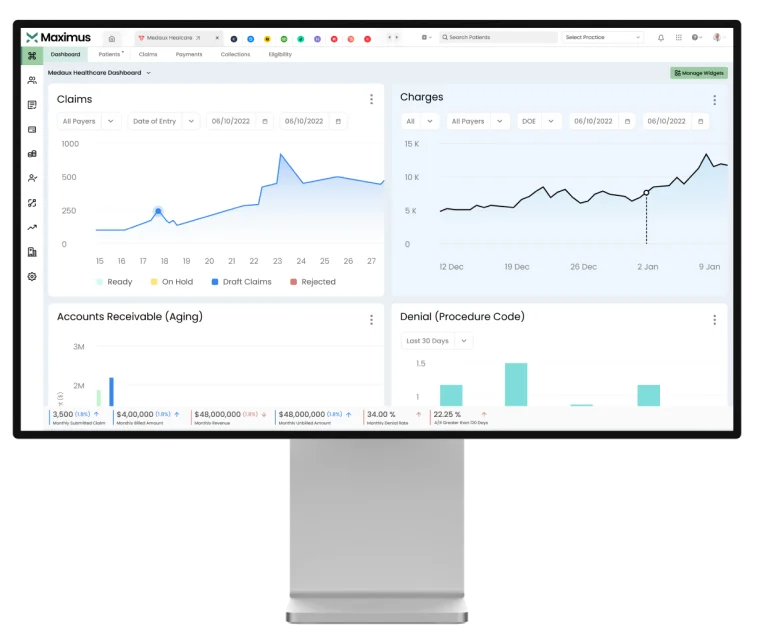
Our AAPC-certified billing and coding team processes up to 75,000 claims daily with accuracy to ensure your practice receives maximum reimbursements.

The MIPS program by Medicare will remain active in 2024, promoting excellent patient care. It evaluates performance across categories such as:
MIPS scores use a weighted system with specific point values and reporting timelines. The requirements can be challenging, but our expertise can help you meet the 75% quality reporting target.

We handle all aspects of verification and renewals so that you can focus on providing exceptional patient care. Our provider credentialing process includes the following steps:


Team up with us to optimize your revenue cycle. Watch your income grow by up to 30% while providing better care for your patients. Contact us now!
Have questions or need support? Feel free to reach out to us anytime. Our team is always ready to assist you with any queries or concerns you may have. Let’s connect and make things easier for you!
(505) 373-0770

Copyright© 2025. All rights reserved. Developed by Websites Developer